Abstract
Mitochondria display complex morphology and movements, which complicates their segmentation and tracking in time-lapse images. Here, we introduce Mitometer, an algorithm for fast, unbiased, and automated segmentation and tracking of mitochondria in live-cell two-dimensional and three-dimensional time-lapse images. Mitometer requires only the pixel size and the time between frames to identify mitochondrial motion and morphology, including fusion and fission events. The segmentation algorithm isolates individual mitochondria via a shape- and size-preserving background removal process. The tracking algorithm links mitochondria via differences in morphological features and displacement, followed by a gap-closing scheme. Using Mitometer, we show that mitochondria of triple-negative breast cancer cells are faster, more directional, and more elongated than those in their receptor-positive counterparts. Furthermore, we show that mitochondrial motility and morphology in breast cancer, but not in normal breast epithelia, correlate with metabolic activity. Mitometer is an unbiased and user-friendly tool that will help resolve fundamental questions regarding mitochondrial form and function.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The authors declare that all data supporting the findings of this study are available in the article and its supplementary information files or from the corresponding author upon reasonable request. Source data are provided with this paper.
Code availability
The Mitometer program is written in MATLAB (MathWorks). The MATLAB GUI Mitometer app and corresponding source code are available as Supplementary Software. The software and updated versions are also freely available online through GitHub at https://github.com/aelefebv/Mitometer, with a direct download link available at https://github.com/aelefebv/Mitometer/archive/refs/heads/main.zip.
Change history
29 April 2022
A Correction to this paper has been published: https://doi.org/10.1038/s41592-022-01506-2
References
Iwata, R., Casimir, P. & Vanderhaeghen, P. Mitochondrial dynamics in postmitotic cells regulate neurogenesis. Science 369, 858–862 (2020).
Federico, A. et al. Mitochondria, oxidative stress and neurodegeneration. J. Neurol. Sci. 322, 254–262 (2012).
Green, D. R. & Reed, J. C. Mitochondria and apoptosis. Science 281, 1309–1312 (1998).
Schiavon, C. R. et al. Actin chromobody imaging reveals sub-organellar actin dynamics. Nat. Methods 17, 917–921 (2020).
Baloh, R. H. Mitochondrial dynamics and peripheral neuropathy. Neuroscientist 14, 12–18 (2008).
Westermann, B. Mitochondrial fusion and fission in cell life and death. Nat. Rev. Mol. Cell Biol. 11, 872–884 (2010).
Pigino, G. et al. Alzheimer’s presenilin 1 mutations impair kinesin-based axonal transport. J. Neurosci. 23, 4499–4508 (2003).
Rui, Y., Tiwari, P., Xie, Z. & Zheng, J. Q. Acute impairment of mitochondrial trafficking by β-amyloid peptides in hippocampal neurons. J. Neurosci. 26, 10480–10487 (2006).
Trushina, E. et al. Mutant huntingtin impairs axonal trafficking in mammalian neurons in vivo and in vitro. Mol. Cell. Biol. 24, 8195–8209 (2004).
Wang, X. et al. PINK1 and Parkin target Miro for phosphorylation and degradation to arrest mitochondrial motility. Cell 147, 893–906 (2011).
Kapitein, L. C. & Hoogenraad, C. C. Building the neuronal microtubule cytoskeleton. Neuron 87, 492–506 (2015).
Waterman-Storer, C. M. Microtubules and microscopes: how the development of light microscopic imaging technologies has contributed to discoveries about microtubule dynamics in living cells. Mol. Biol. Cell 9, 3263–3271 (1998).
Caino, M. C. et al. Syntaphilin controls a mitochondrial rheostat for proliferation–motility decisions in cancer. J. Clin. Invest. 127, 3755–3769 (2017).
Caino, M. C. et al. A neuronal network of mitochondrial dynamics regulates metastasis. Nat. Commun. 7, 13730 (2016).
Cheezum, M. K., Walker, W. F. & Guilford, W. H. Quantitative comparison of algorithms for tracking single fluorescent particles. Biophys. J. 81, 2378–2388 (2001).
Yang, Y. et al. Label-free tracking of single organelle transportation in cells with nanometer precision using a plasmonic imaging technique. Small 11, 2878–2884 (2015).
Tinevez, J.-Y. et al. TrackMate: an open and extensible platform for single-particle tracking. Methods 115, 80–90 (2017).
Fischer, C. A. et al. MitoSegNet: easy-to-use deep learning segmentation for analyzing mitochondrial morphology. iScience 23, 101601 (2020).
Falk, T. et al. U-Net: deep learning for cell counting, detection, and morphometry. Nat. Methods 16, 67–70 (2019).
Isensee, F., Jaeger, P. F., Kohl, S. A. A., Petersen, J. & Maier-Hein, K. H. nnU-Net: a self-configuring method for deep learning-based biomedical image segmentation. Nat. Methods 18, 203–211 (2021).
Miller, K. E., Liu, X.-A. & Puthanveettil, S. V. Automated measurement of fast mitochondrial transport in neurons. Front. Cell. Neurosci. 9, 435 (2015).
Alsina, A. et al. Real-time subpixel-accuracy tracking of single mitochondria in neurons reveals heterogeneous mitochondrial motion. Biochem. Biophys. Res. Commun. 493, 776–782 (2017).
Vallmitjana, A., Civera-Tregon, A., Hoenicka, J., Palau, F. & Benitez, R. Motion estimation of subcellular structures from fluorescence microscopy images. Annu. Int. Conf. IEEE Eng. Med. Biol. Soc. 2017, 4419–4422 (2017).
Winter, M. R., Fang, C., Banker, G., Roysam, B. & Cohen, A. R. Axonal transport analysis using multitemporal association tracking. Int. J. Comput. Biol. Drug Des. 5, 35–48 (2012).
Kandel, J., Chou, P. & Eckmann, D. M. Automated detection of whole-cell mitochondrial motility and its dependence on cytoarchitectural integrity. Biotechnol. Bioeng. 112, 1395–1405 (2015).
Giedt, R. J., Pfeiffer, D. R., Matzavinos, A., Kao, C.-Y. & Alevriadou, B. R. Mitochondrial dynamics and motility inside living vascular endothelial cells: role of bioenergetics. Ann. Biomed. Eng. 40, 1903–1916 (2012).
Valente, A. J., Maddalena, L. A., Robb, E. L., Moradi, F. & Stuart, J. A. A simple ImageJ macro tool for analyzing mitochondrial network morphology in mammalian cell culture. Acta Histochem. 119, 315–326 (2017).
Viana, M. P., Lim, S. & Rafelski, S. M. Quantifying mitochondrial content in living cells. Methods Cell Biol. 125, 77–93 (2015).
Lihavainen, E., Mäkelä, J., Spelbrink, J. N. & Ribeiro, A. S. Mytoe: automatic analysis of mitochondrial dynamics. Bioinformatics 28, 1050–1051 (2012).
Klopfenstein, D. R. & Vale, R. D. The lipid binding pleckstrin homology domain in UNC-104 kinesin is necessary for synaptic vesicle transport in Caenorhabditis elegans. Mol. Biol. Cell 15, 3729–3739 (2004).
Pilling, A. D., Horiuchi, D., Lively, C. M. & Saxton, W. M. Kinesin-1 and Dynein are the primary motors for fast transport of mitochondria in Drosophila motor axons. Mol. Biol. Cell 17, 2057–2068 (2006).
Chang, C.-R. & Blackstone, C. Dynamic regulation of mitochondrial fission through modification of the dynamin-related protein Drp1. Ann. NY Acad. Sci. 1201, 34–39 (2010).
Ploumi, C., Daskalaki, I. & Tavernarakis, N. Mitochondrial biogenesis and clearance: a balancing act. FEBS J. 284, 183–195 (2017).
McCarron, J. G. et al. From structure to function: mitochondrial morphology, motion and shaping in vascular smooth muscle. J. Vasc. Res. 50, 357–371 (2013).
Smal, I., Draegestein, K., Galjart, N., Niessen, W. & Meijering, E. Particle filtering for multiple object tracking in dynamic fluorescence microscopy images: application to microtubule growth analysis. IEEE Trans. Med. Imaging 27, 789–804 (2008).
Dorn, J. F., Danuser, G. & Yang, G. Computational processing and analysis of dynamic fluorescence image data. Methods Cell Biol. 85, 497–538 (2008).
Huth, J. et al. Significantly improved precision of cell migration analysis in time-lapse video microscopy through use of a fully automated tracking system. BMC Cell Biol. 11, 24 (2010).
Vasquez, R. J., Howell, B., Yvon, A. M., Wadsworth, P. & Cassimeris, L. Nanomolar concentrations of nocodazole alter microtubule dynamic instability in vivo and in vitro. Mol. Biol. Cell 8, 973–985 (1997).
Heggeness, M. H., Simon, M. & Singer, S. J. Association of mitochondria with microtubules in cultured cells. Proc. Natl Acad. Sci. USA 75, 3863–3866 (1978).
Rambold, A. S., Kostelecky, B., Elia, N. & Lippincott-Schwartz, J. Tubular network formation protects mitochondria from autophagosomal degradation during nutrient starvation. Proc. Natl Acad. Sci. USA 108, 10190–10195 (2011).
Leonard, A. P. et al. Quantitative analysis of mitochondrial morphology and membrane potential in living cells using high-content imaging, machine learning, and morphological binning. Biochim. Biophys. Acta 1853, 348–360 (2015).
Gomes, L. C., Di Benedetto, G. & Scorrano, L. During autophagy mitochondria elongate, are spared from degradation and sustain cell viability. Nat. Cell Biol. 13, 589–598 (2011).
DeRose, Y. S. et al. Tumor grafts derived from women with breast cancer authentically reflect tumor pathology, growth, metastasis and disease outcomes. Nat. Med. 17, 1514–1520 (2011).
Ma, D. et al. Patient-derived xenograft culture-transplant system for investigation of human breast cancer metastasis. Preprint at bioRxiv https://doi.org/10.1101/2020.06.25.172056 (2020).
Wu, P.-H., Giri, A., Sun, S. X. & Wirtz, D. Three-dimensional cell migration does not follow a random walk. Proc. Natl Acad. Sci. USA 111, 3949–3954 (2014).
Zhao, J. et al. Mitochondrial dynamics regulates migration and invasion of breast cancer cells. Oncogene 32, 4814–4824 (2013).
Walker, J. E. The ATP synthase: the understood, the uncertain and the unknown. Biochem. Soc. Trans. 41, 1–16 (2013).
Pedregosa, F. et al. Scikit-learn: machine learning in Python. J. Mach. Learn. Res. 12, 2825–2830 (2011).
Digman, M. A., Caiolfa, V. R., Zamai, M. & Gratton, E. The phasor approach to fluorescence lifetime imaging analysis. Biophys. J. 94, L14–L16 (2008).
Bird, D. K. et al. Metabolic mapping of MCF10A human breast cells via multiphoton fluorescence lifetime imaging of the coenzyme NADH. Cancer Res. 65, 8766–8773 (2005).
Stringari, C. et al. Phasor approach to fluorescence lifetime microscopy distinguishes different metabolic states of germ cells in a live tissue. Proc. Natl Acad. Sci. USA 108, 13582–13587 (2011).
Scaduto, R. C. & Grotyohann, L. W. Measurement of mitochondrial membrane potential using fluorescent rhodamine derivatives. Biophys. J. 76, 469–477 (1999).
Will, Y., Hynes, J., Ogurtsov, V. I. & Papkovsky, D. B. Analysis of mitochondrial function using phosphorescent oxygen-sensitive probes. Nat. Protoc. 1, 2563–2572 (2006).
Arai, S. et al. Mitochondria-targeted fluorescent thermometer monitors intracellular temperature gradient. Chem. Commun. (Camb.) 51, 8044–8047 (2015).
Lee, M. H. et al. Mitochondria-immobilized pH-sensitive off–on fluorescent probe. J. Am. Chem. Soc. 136, 14136–14142 (2014).
Nguyen, Q. H. et al. Profiling human breast epithelial cells using single cell RNA sequencing identifies cell diversity. Nat. Commun. 9, 2028 (2018).
Acknowledgements
The authors thank F. Adame and M. Li for much of the cell culture work, and F. Palomba, A. Vallmitjana and L. Scipioni for thoughtful feedback on experimental design and careful review of the manuscript. The authors also thank E. Gratton for helpful discussions and advice on the application of Mitometer to metabolic analysis of single mitochondria; G. A. Hernandez for her technical assistance with processing human mammary samples for this project; and A. Welm at the Huntsman Cancer Institute, Salt Lake City, Utah for generously providing PDX models used in this study. R. Waymack from the laboratory of Z. Wunderlich at University of California, Irvine is thanked for the help on imaging with the Nikon Eclipse Ti-E. Image and data acquisition were made possible through access to the Laboratory for Fluorescence Dynamics, a shared resource center supported by the National Institutes of Health (grant no. P41-GM103540). This study was supported by funds from the National Science Foundation (grant nos. DMS1763272 and 1847005 to M.A.D. and NSF GRFP DGE-1839285 to A.E.Y.T.L.), a grant from the Simons Foundation (594598 QN), by funds from the National Institutes of Health and the National Cancer Institute (1R01CA234496 to K.K.; K22 CA190511 to D.A.L.), the American Cancer Society (132551-RSG-18-194-01-DDC to K.K.), and the V Foundation (V2019-019 to D.A.L.). D.M. was supported by the Canadian Institutes of Health Research Postdoctoral Fellowship. This work was also supported in part by American Cancer Society Institutional Research Grant 134045-IRG-19-145-16-IRG.
Author information
Authors and Affiliations
Contributions
A.E.Y.T.L. initiated the study, designed and implemented the Mitometer software, designed and performed cellular imaging experiments and analysis, and wrote the manuscript. D.M. designed the experiments, prepared and cultured the 3D primary samples and cell lines for the breast cancer and non-malignant breast cell experiments, and extensively reviewed and edited the manuscript. K.K. and D.A.L. helped review and edit the manuscript. M.A.D. initiated the study, supervised the research, and helped review and edit the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information Nature Methods thanks Carsten Marr and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Rita Strack was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Diffuse background removal surrounding objects of complex shapes.
Circular median filters of diameters of 0.6 μm (a) to 2 μm (c) (corresponding to the minimum area threshold and a value larger than the minor axis length of mitochondria) in 1-pixel increments (b) are convolved with the original image. Close-ups of regions with high (i) and low (i) diffuse background noise convolved with a small (d) medium (e) and large (f) median filter (left), with corresponding minimum median filter values at each filter size (right). g, The minimum value of each pixel in the stack of median filtered images (which also contains the original image) is used to build the diffuse background image, showing high diffuse noise in the dense regions (i) and minimal diffuse noise in the sparse regions (ii). h, The diffuse background image is then subtracted from the original image to produce a diffuse background subtracted image, separating adjacent mitochondria in dense regions (i) and keeping mitochondria intact in sparse regions (ii).
Extended Data Fig. 2 Parameter exploration for choosing low-pass filter and threshold parameters.
a, The diffuse background subtracted (-DB) image is taken as an input. b, The output is an image with optimal parameters (e) chosen to segment mitochondrial objects and remove noise. A mismatch in parameters results in high noise (c), false connections and area overestimation (d), and loose connections (leading to high variability) with area overestimation (f). The parameters are chosen based on the z score normalized addition of 3 features: the variability in the median area of the mitochondria between temporal frames (g), the variability in the number of mitochondria found between temporal frames (h), and ½ the negative number of mitochondria found between temporal frames (i). We give less weight to the number of mitochondria found as many false disconnections biases the parameter selection towards a highly thresholded image, while noise biases the parameter selection towards a non-thresholded image. This addition results in the cost function used for minimization to select optimal parameters, which we run through a symmetrically padded 3×3 median filter to ensure selected parameters are in a region of low cost, rather than an outlying point (j). Colored dots represent parameters chosen to create images shown in c-f with respective border colors. Colors in c-f represent randomly pseudocolored connected components.
Extended Data Fig. 3 Flowchart for morphology and displacement-based global cost minimization tracking.
a, A matrix of intensity weighted centroid distances is built comprised of the difference between every existing track (columns) and every mitochondrion found in the current time frame (rows). A region of mitochondria from an adjacent cell can be seen in the dotted white area, resulting in large differences between the mitochondria of the two cells. b, A mask is created to avoid assignments between any mitochondria and track which are further than 3 frames apart (the maximum search time threshold), and at a distance greater than 1 μm multiplied by the frame time apart (the maximum velocity threshold). c, The mask is applied to the difference matrices of all mitochondrial features and distance. d, The difference matrices are then squared, z score normalized, weighted, and summed to create the final difference matrix (e). f, A diagonal matrix of new track costs is appended to the difference matrix to allow newly found mitochondria to be assigned to a new track. g, Every mitochondrion (row) in the matrix is assigned to a single track (column) that leads to a globally minimized cost of assignment. h, A mitochondrion which is assigned to a track that also corresponds to its own individually minimum cost is labelled as a confident assignment. i, This process is repeated for all temporal frames. All confident tracks are then analyzed for interCoV:intraCoV ratios for each mitochondrial morphological feature, and weights are set accordingly. These weights are used to rerun the tracking algorithm, leading to a higher number of mitochondria that are confidently tracked for the full length of the time stack (j) and to less total number of tracks overall (k).
Extended Data Fig. 4 Flowchart for gap-closing scheme.
a, A matrix of differences between all new tracks’ first frame number and all lost tracks’ last frame number. b, The frame difference matrix is thresholded based a maximum search time threshold of 15 seconds to create a mask. c, The mask is applied to the matrix of the intensity weighted centroid distances between the new tracks’ first centroid position and last tracks’ last centroid position. d, The distance matrix is thresholded based on the maximum velocity threshold of 1 μm/s. e, Any gap closure resulting in a travel angle coefficient of variation under 0.2 is removed. f, The final masked gap closing matrix is produced, which is then globally minimized to assign new tracks with possible lost track candidates. g, The gap-closing scheme is repeated in its entirety until the total number of tracks stabilizes. In this example, it took 4 iterations to stabilize to 469 tracks.
Extended Data Fig. 5 Live-cell time lapse images with added noise.
The comparison of area (a) and speed (b) of mitochondria in live-cell time lapse images of PC12 (i), H1299 (ii), and HFF (iii) cells between the original image and images with added noise to simulate a lower full well depth (Poissonian noise) and higher read noise root mean square (RMS) value (Gaussian noise). Comparisons are done via a two-sided Wilcoxon rank sum test. c, Representative images of TMRM labelled H1299 cells with simulated noise corresponding to the numbers in panels ii. N = 3 time lapse images per cell line.
Extended Data Fig. 6 Three-dimensional spheroid cultures.
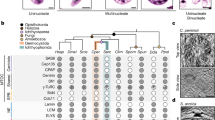
a Representative images of human reduction mammoplasty samples (Patient 72, Patient 76, Patient 08, Patient 99, Patient 97), established breast cancer cell lines (MCF-7, T-47D, MDA-MB-231, MDA-MB-468, BT-549), and patient derived xenografts (HCI-010, HCI-002) embedded in Matrigel and grown in three-dimensional spheroid culture. Gray = brightfield, cyan = mitochondria fluorescence (TMRM), pink = nuclear fluorescence (NucBlue).
Supplementary information
Supplementary Information
Supplementary Notes 1–15 with their corresponding figures and tables.
Supplementary Data 1
SN-1_1_Data.
Supplementary Data 2
SN-1_2_Data.
Supplementary Data 3
SN-5_1_Data.
Supplementary Data 4
SN-9_1_Data.
Supplementary Data 5
SN-12_1_Data.
Supplementary Video 1
Supp_Vid1.
Supplementary Video 2
Supp_Vid2.
Supplementary Video 3
Supp_Vid3.
Supplementary Video 4
Supp_Vid4.
Source data
Source Data Fig. 3
In silico validation statistical source data.
Source Data Fig. 4
In vitro validation statistical source data.
Source Data Fig. 5
Breast cell mitochondria and random forest statistical source data.
Source Data Fig. 6
Breast cell Mitometer and NADH FLIM statistical source data.
Source Data Extended Data Fig. 5
Simulated full read noise and RMS noise statistical source data.
Rights and permissions
About this article
Cite this article
Lefebvre, A.E.Y.T., Ma, D., Kessenbrock, K. et al. Automated segmentation and tracking of mitochondria in live-cell time-lapse images. Nat Methods 18, 1091–1102 (2021). https://doi.org/10.1038/s41592-021-01234-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41592-021-01234-z
This article is cited by
-
Elevated SLC7A2 expression is associated with an abnormal neuroinflammatory response and nitrosative stress in Huntington’s disease
Journal of Neuroinflammation (2024)
-
Nano-flow cytometry unveils mitochondrial permeability transition process and multi-pathway cell death induction for cancer therapy
Cell Death Discovery (2024)
-
Mitochondrial Transplantation in Ischemic Stroke: Insights from a First-in-Human Brain Trial
Current Transplantation Reports (2024)
-
Mitochondrial modulation with leriglitazone as a potential treatment for Rett syndrome
Journal of Translational Medicine (2023)
-
Amyloid-β accumulation in human astrocytes induces mitochondrial disruption and changed energy metabolism
Journal of Neuroinflammation (2023)